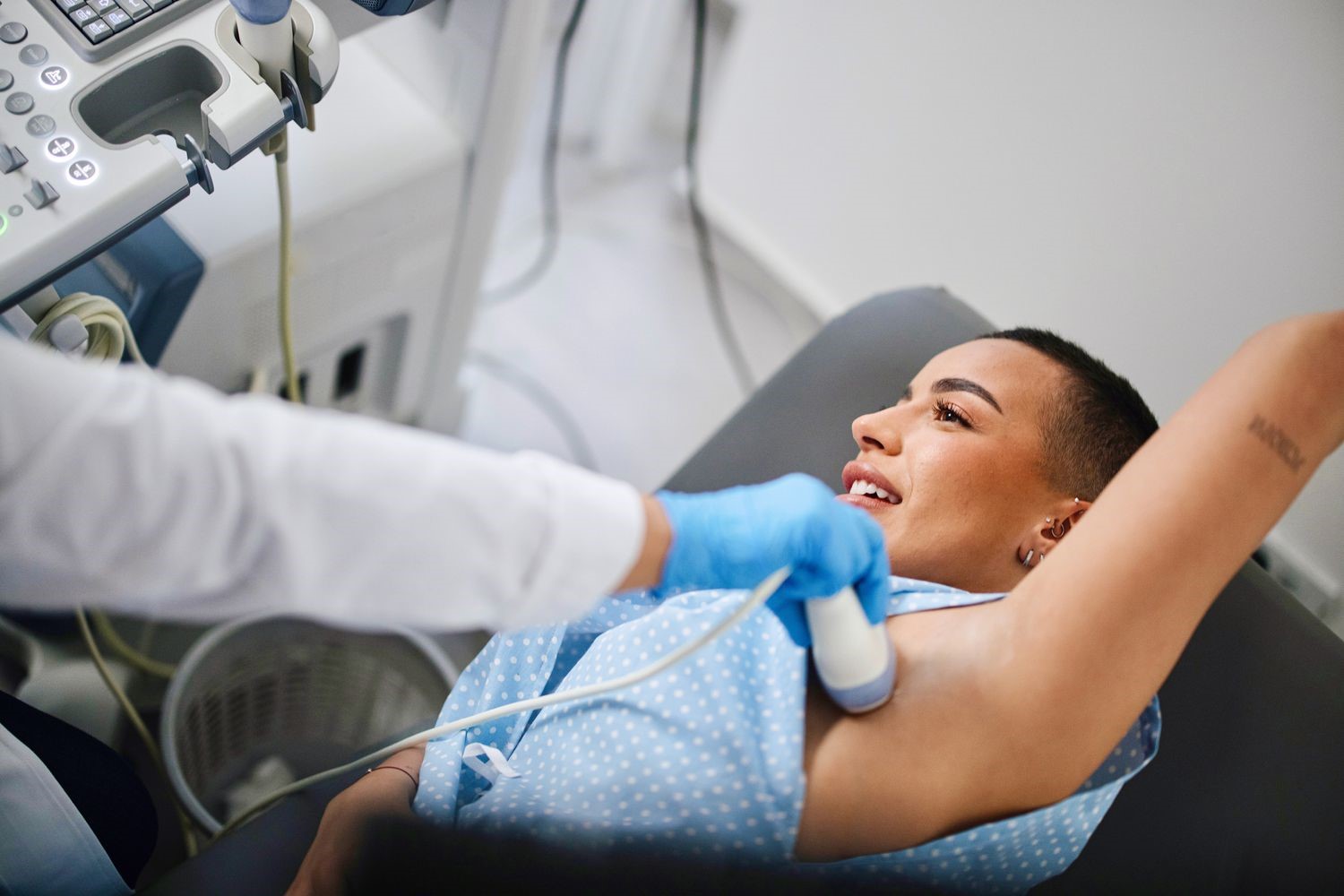
An important percentage of patients—about 21%—say that they would miss follow-up breast imaging after an abnormal mammogram if they had to pay a deductible, new research exhibits. The study, posted on April 4 in Radiology, asked about 700 participants if, in a hypothetical situation, they would forgo more imaging to confirm whether they had breast cancer. The high ratio of individuals who said they would show how the cost is often a deterrent for breast cancer screenings and diagnoses, specialists said.
Here’s what professionals had to say about why such a substantial portion of patients may be missing breast cancer imaging, why that’s the reason for anxiety, and what to do at the beginning of high expenses.
Extra Costs Deter Somebody From Seeking Breast Cancer Imaging
Now, if a person goes in to get a mammogram, it will most likely be at no cost to them. This is where items can get pricey.
Except for those who gave a yes or no to each theoretical report, a substantial portion of individuals said they weren’t certain what they would do—another 20% said they were uncertain about whether they would skip a follow-up imaging after an irregular mammogram and 16% said they didn’t know if they would cut initial mammography.
This could mean that the actual digit of individuals who end up bypassing these follow-up tests and screenings is even more elevated.
The analysis does have a few rules, experts presented. Since there were only a few hundred parties, the effects may not echo the views of the entire U.S. residents who are qualified for mammograms. Also, the students asked patients to describe their conduct in a theoretical case, which could mean they’d act differently when confronted with an actual strange mammogram and a high deductible.
Nevertheless, the study’s results appear to be in line with what students already comprehend. An analysis issued last year found that about 20% of individuals did not produce for their follow-up study after obtaining inconclusive mammogram outcomes. The issue is clear outside of breast cancer screening, too—about 40% of survey respondents said cutting a suggested medical test or medicine because they were nervous about the cost.
The Significance of Follow-Up Imaging for Early Detection
Accepting abnormal mammogram effects is relatively common, said Therese Bevers, MD, medical head of the Cancer Prevention Center at the University of Texas MD Anderson Cancer Center. But it’s still better to be secure.
Where do the two cross? How many of the 20% of breast cancers are going to be in that one of five ladies who select to not get the other workup?
This is exactly what healthcare providers are trying to avoid, Sinaiko demonstrated.
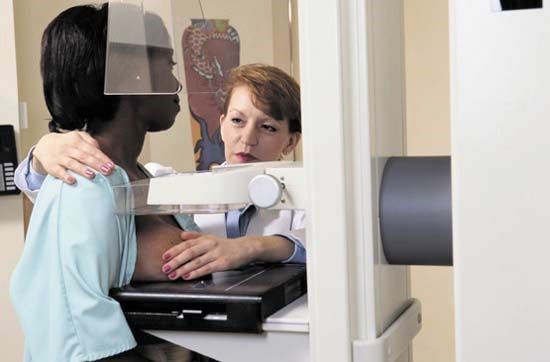
“Cancer results are a lot better than before it is seen,” she said. “We want patients to go for their mammograms to be filtered so that we can see the condition as early as possible, then it just shows to better survival and quality of life.”
The results are also concerning because they present the question of whether skipping care is common practice even after people are diagnosed with breast cancer, told Sarah Tevis, MD, assistant teacher of surgery at the University of Colorado Anschutz Medical Campus.
What Individuals Can Do to Get Their Breast Imaging Costs Down
Though people ought to devote themselves to other breast cancer imaging if required, it can be hard to quantify the cost. For one, the cost often counts on the type of mirroring provider orders, the specialists said.
“They could maybe just require a diagnostic mammogram that soothes the radiologist that there’s nothing concerning going on,” Dr. Tevis said. “Or they could need a mammogram and an ultrasound and a biopsy and an MRI.”
What the patients themselves are liable for paying also relies on whether they have health insurance and the type they have.
If the additional breast imaging fails under someone’s deductible, Sinaiko defined, they will have to pay the full cost. It may be less costly if an individual has a copay or coinsurance, where they’ll pay a flat fee or a percentage of the cost, respectively.

“As you start to think about the financial obstacles to getting that further workup, you can see why some ladies may find that prohibitive.